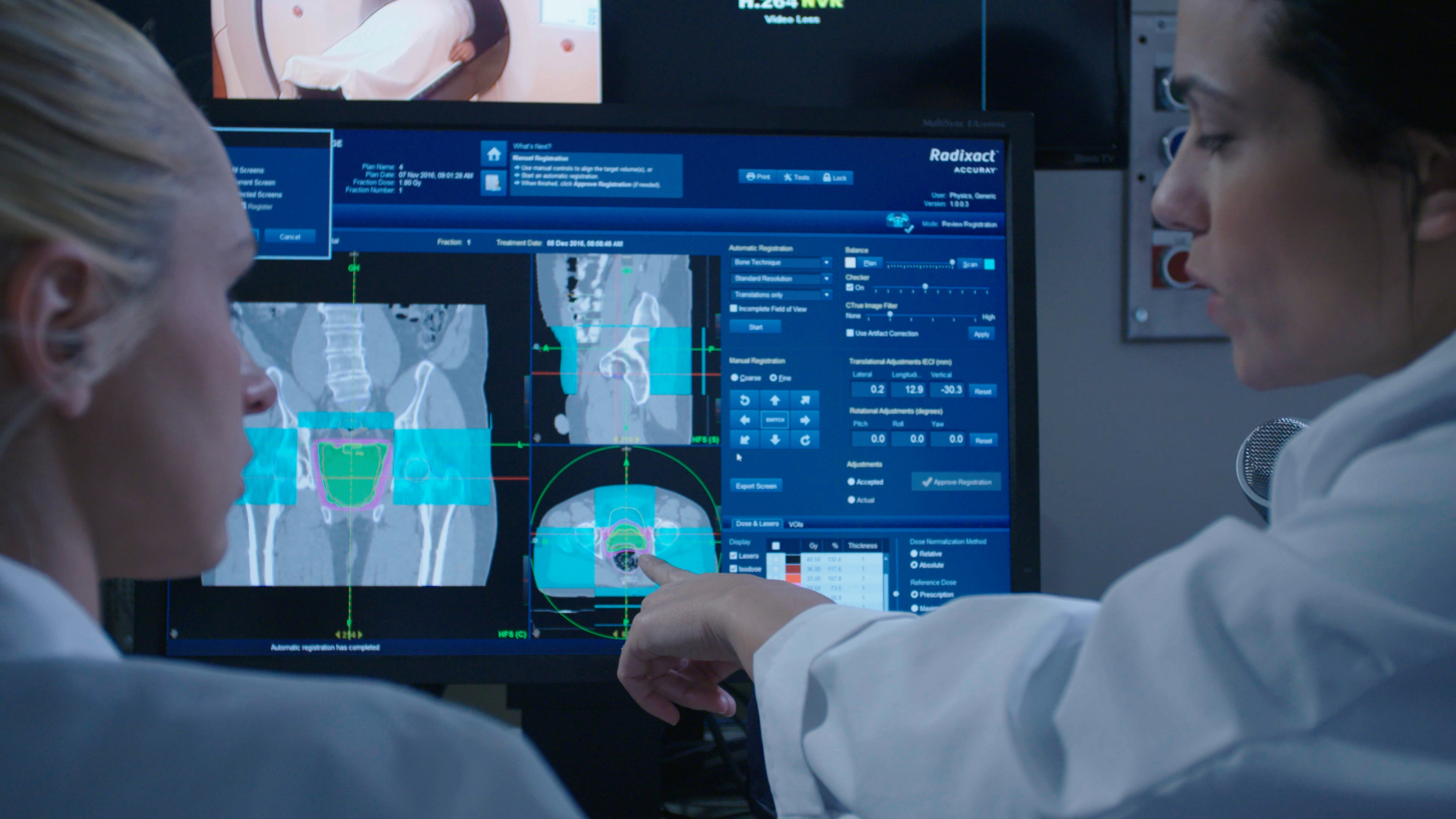
The TomoTherapy Radixact treatment delivery system design provides volumetric beam delivery. This customized design combined with next generation CT fusion imaging provides state of the art cancer treatment for patients.
Radiation therapy uses a special type of very high-energy X-rays to destroy cancer cells and shrink tumors. In order to give the patient the most effective treatment options. MC Radiation Oncology Center offers a complete array of radiation oncology services using long established conventional approaches to the most robust methods available. We consider the advantage of every treatment device and technique when deciding on the optimal treatment approach for each patient. We select treatment delivery options that target tumors precisely.
Optimal and precise treatment plans afford impact, while minimizing damage to critical structures and healthy tissue. As mentioned above, radiation therapy for cancer uses high-energy Xray beams, so our patients will feel no pain during treatment. Although the therapy is generally not painful, the equipment used during planning and treatment can be scary to some. Our health care team will provide a safe and comfortable experience roughout your treatment.
In order to provide the safest and most effective treatment, radiation therapy is delivered in many small doses over a period of time. Most patients require brief treatment sessions five days a week for several weeks.
GENERAL QUESTIONS ABOUT CANCER TREATMENT
COMMON QUESTIONS ABOUT RADIATION THERAPY
• What is radiation therapy?
Radiation therapy is an effective cancer treatment that uses an external or internal radiation source to destroy cancer cells. It may be used alone or in combination with other forms of cancer treatment including surgery and chemotherapy.
• How does it work?
Radiation therapy works by destroying cancerous cells and shrinking tumors. There are two basic types of radiation therapy: External Beam Radiation Therapy (EBRT) and Internal Radiation Therapy also called Brachytherapy with EBRT, the radiation is delivered from outside of the body using one of several different types of radiation systems. For patients undergoing Brachytherapy, a radioactive source is temporarily or permanently implanted inside the body either in the tumor site or in a cavity left by a tumor that has been surgically removed.
Regardless of whether you and your Radiation Oncologist choose a form of External Beam Radiation Therapy or Brachytherapy, the primary objective of these increasingly sophisticated systems is to deliver as much radiation as possible — for maximum effectiveness — while minimizing damage to surrounding healthy tissue and possible side effects.
• Can radiation therapy effectively treat my cancer?
Radiation is an effective treatment for cancer as well as an effective therapy for shrinking and managing the disease. Success rates depend on the type of cancer, its stage and its location.
• How long does radiation therapy take?
The length of a radiation treatment program depends on the type of radiation therapy chosen as well as the stage, size and location of the disease. Some radiation therapies require just a few sessions while others may require daily visits for a number of weeks. Each appointment typically lasts from a few minutes up to half an hour.
• What are the most common side effects of radiation therapy?
With the increased sophistication and precision of radiation therapy technology, the extent of side effects has been significantly reduced. Some patients experience side effects while others do not. The type and severity of side effects from radiation typically depends on the location of the tumor. The most common side effects are nausea, fatigue, swelling, loss of appetite and skin irritation. Most of these disappear within a few weeks after treatment is completed. At 21st Century Oncology, our treatment teams are very skilled at helping patients manage side effects and minimize their severity.
• Is radiation therapy painful?
External Beam Radiation Therapy (EBRT) is painless. There may be slight discomfort if you have to have markers implanted to help target the beam or if you have stereotactic radio surgery and must be fitted with a head frame. Internal Radiation or Brachytherapy is generally not painful although there may be some slight discomfort after the radiation source is implanted.
• Can I drive myself to and from treatments?
External Beam Radiation Therapy, regardless of the technology and therapy type, does not require sedation. You will be able to drive yourself although we do recommend you bring a friend or family member to treatments as a second set of eyes and ears. Some forms of High Dose Rate Brachytherapy, such as Accelerated Partial Breast Irradiation do not require sedation, but others do. Low Dose-Rate Brachytherapy is a surgical procedure, which is typically done in an outpatient setting. That said, we recommend you bring someone with you to your appointments.
• Is radiation therapy safe?
It is common for patients to be concerned about being treated with radiation. Today’s systems are extremely safe and meticulously tested and maintained. At MC Radiation Oncology Center, we take safety to a new level with multiple safety checks automatically measures each dosage amount against the patient’s treatment plan. The Radiation Therapist check for accuracy and if there are any discrepancies before moving forward with treatment. The Therapist also check you position by taking state of the art images and if there is a change in your position, they will make the final adjustments prior to delivering your treatment. Patients going through radiation therapy are not a danger to others although patients that undergo low dose-rate Brachytherapy are advised to stay away from women who are pregnant and babies for several days. With time the radiation source diminishes and becomes non-radioactive.
The MC Radiation Therapy Process
The process of radiation therapy will be customized for our patients, depending on which form of radiation therapy patients and their physicians choose as their options. Overall, there are five basic steps of radiation therapy that we can share to give patients an idea of what to expect.
These are the steps followed by MC Radiation Oncology Center; Initial consultation, simulation, treatment planning, treatment delivery, weekly management and post treatment follow-up.
Step 1: Initial consultation
Consultation is the first step of the radiation therapy process. This involves an appointment with a radiation oncologist, who reviews a patient’s medical records, pathology reports and radiology images and performs a physical examination. Based on this review, The specific radiation therapy treatment is chosen for the patient and they will be offered an appointment for simulation.
Step 2: Treatment Setup or Simulation at MC Radiation
A special CT scan (called CT/Simulation) is acquired for every patient. Your physicians use the scans to identify the size, shape and location of the lesion/tumor along with the surrounding vital structures to be avoided.
You will be placed in the treatment position, and often there will be customized “immobilization” devices such as mesh masks, headrests, or form-fit body molds to maintain your body position the same on a day to day basis. Sometimes, the area on your body that requires treatment will be marked with a tiny tattoo “dot”. This will help with the treatment set and ensure that the radiation is directed properly each day. The process is simple and painless.
Step 3: Treatment Planning
Your previously obtained CT scan and data are sent to the treatment-planning computer system where the physicians’ team will use advanced software to customize the radiation beams that will be delivered to the tumor or lesion during your treatment. Treatment plans are customized for each patient and become the blueprint for treatment delivery. Developing the treatment plan may be a complex process aided by the use of computers that recreate your “virtual anatomy” and location of your cancer or tumor. It may take several days to complete the treatment planning process. You do not need to be present during this step.
Step 4: Treatment Delivery
The number of treatments vary depending and per diagnosis (between 1 and 35 daily treatments).
Arriving – Wear comfortable clothing and no jewelry. You may bring your favorite music to listen to during the treatment. Try to relax knowing this will be a painless procedure. Feel free to bring a list of questions to ask the radiation team. We are here to ensure your comfort and safety.
Positioning.
You will be asked to lie on the treatment table and will be fitted with the custom mask or body mold made for you earlier during the set-up process. In some cases a mild sedative will be given to you to help you relax.
Painless Treatment
During treatment, you will need to lie still. The length of treatment varies depending on the location of your lesion/tumor. The image guidance system periodically compares x-ray images to the CT scan to ensure the radiation is targeted accurately at the tumor.
Step 5: Weekly patient management
Over the course of radiation therapy, you will meet with your doctor at least once a week as well as the other members of the treatment team, including nurses. In addition, should you have concerns or symptoms that need to be addressed, you may meet with any of your treatment team members on any day at your request.
Completion
When your treatment sessions are completed, our nursing staff will do an assessment and once completed you will be released to go home and may resume normal activity.
Step 6: Post Treatment Follow-up
Upon completion of your treatment, a follow-up appointment will be scheduled to monitor the recovery and overall health of our patients. Additional diagnostic tests may be ordered. Reports on the status of our patients are sent to all physicians involved in patient care. As time goes by, the frequency of visits to the Department of Radiation Oncology will decrease, but physicians and other providers are always available to talk with patients and address any questions and concerns they may have.